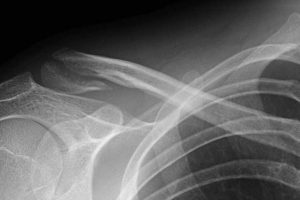
Many conditions affect the body’s musculoskeletal system.
While mild cases will respond to home care remedies, others will require the help and expertise of an orthopaedic specialist.
Some of the most prevalent orthopaedic disorders include:
Osteoarthritis
Considered the most common type of arthritis, osteoarthritis is a chronic degenerative joint disease that often affects old and middle-aged individuals.
The condition is characterized by the breaking down of the joint cartilage.
While osteoarthritis can develop in any joint, it usually affects the knees, hands, spine, and hips.
Causes
Osteoarthritis has two classifications—primary and secondary.
The former has no known cause while the latter can be attributed to other factors like infection, deformity, injury, or another disease.
The condition starts with the breakdown of the cartilage.
As it breaks down, the ends of the bone may thicken and bony growths (spurs) can form.
These spurs can interfere with joint movement and bits of bone and cartilage can end up floating in the joint space.
In addition, fluid-filled cysts may also develop in the bone resulting in limited joint movement.
Symptoms
The most prevalent indicator of the condition is pain after joint overuse or inactivity.
Symptoms of osteoarthritis often gradually develop over the years.
Symptoms may vary from one individual to another.
However, it can often include the following:
- Joint pain
- Joint stiffness (especially noticeable after inactivity or sleep)
- Limited joint movement
- Grinding feeling especially when the joint is moved (more prevalent in the advanced stages)
Treatment
Treatment of the condition will often depend on the patient’s age, symptoms, and general health.
The severity of the condition will also be taken into account.
Treatment goals include reducing joint stiffness and pain and improving joint mobility.
Treatment interventions can include:
- Exercise – regular exercise (including strengthening and stretching) can help minimize pain and other symptoms.
- Heat treatment – treating the joint affected with heat may be helpful in alleviating pain.
- Occupational and physical therapy – these types of therapy may help improve flexibility, minimize joint strain, and reduce joint pain.
- Assistive devices like splints may also be beneficial.
- Weight maintenance – maintaining a healthy weight can help minimize symptoms.
- Medications – this can include anti-inflammatory medications and pain relievers.
- Joint surgery – surgery might be recommended when there is severe joint damage.
Fractures
A partial or complete break in the bone is called a fracture.
Fractures are classified as open or closed.
Open fractures (compound) occurs when the bone pokes through the skin or when a deep wound exposes the bone.
Closed fractures (simple) occurs when the bone is broken but the skin stays intact.
There are different types of fractures.
Some of the most common include:
- Greenstick – a bone portion breaks causing the other side to bend
- Transverse – the break is in a straight line (across the bone)
- Spiral – break spirals around the bone (usually in twisting injuries)
- Oblique – break is diagonal across the bone
- Compression – bone is crushed
- Segmental – bone is fractured in two places
- Comminuted – bone is broken into three (or more) pieces, with bone fragments present in the site of the fracture
Causes
Fractures often occur when the force applied to the bone is more than it can handle.
Bone fractures can be attributed to trauma and falls.
It can also be a result of a kick or direct blow to the body.
Repetitive motions and overuse can also tire muscles and put strain and pressure on the bone. This can result in stress fractures—a condition common among athletes.
Fractures can also occur as a result of diseases that weaken the bone, like bone cancer or osteoporosis.
Symptoms
While fracture symptoms can vary, some of the most common include:
- Sudden pain
- Difficulty moving or using the affected area or the joints nearby
- Swelling
- Noticeable deformity
- Redness, warmth, and bruising
Treatment
Treatment goals for fracture include putting the broken pieces back in place, preventing complications, controlling the pain, restoring normal function, and giving the affected bone time to heal.
Treatment options can include:
- Cast or splint – used to immobilize the affected area in order to keep the bone aligned. It also helps ensure the injured area is kept from motion or use while the affected bone is still healing.
- Medicine – medications are given to control pain.
- Traction – pulleys, weights, strings, and a metal frame is attached on or over the bed in order to stretch the tendons and the muscles around the broken bone. It will help the affected bone align and heal.
- Surgery – surgery might be recommended to put the broken bones back in place. Internal or external fixation devices may be used to hold the bone fragments together while healing.
Carpal Tunnel Syndrome
When the median nerve is compressed while it passes through the carpal tunnel, carpal tunnel syndrome occurs.
The median nerve functions by providing motor and sensory functions to the 3 middle fingers and the thumb.
Women are 3 times more prone to developing the condition compared to men.
Causes
Most cases of the condition cannot be attributed to a specific cause.
However, the following are some of the factors that may contribute to the development of the condition:
- Constant, repetitive, and small movements using the hands (i.e. using a keyboard or typing)
- Repetitive, frequent, and grasping hand movements (in sports or when doing certain physical activities)
- Metabolic or hormonal changes (i.e. pregnancy, menopause, or thyroid imbalance)
- Blood sugar level changes (for instance, in type 2 diabetes)
- Other wrist injuries or conditions (i.e. sprain, dislocation, break, strain, and inflammation)
- History of carpal tunnel syndrome in the family
Symptoms
Some of the telltale indicators of carpal tunnel syndrome include:
- Weakness when gripping objects (either with one or both hands)
- Numbness or pain (in one or both hands)
- “Pins and needles” sensation in the fingers
- Swollen feeling in the affected fingers
- Tingling or burning in the fingers (especially in the index and middle fingers and the thumb)
- Numbness and pain that worsens at night and may even interrupt sleep
Treatment
An orthopaedic specialist can recommend the best treatment intervention for the condition based on the following:
- Patient’s age
- Patient’s medical history
- Patient’s overall health
- Severity of the condition
- Patient’s tolerance to specific medications, therapies, or procedures
- Patient opinion or preference
Treatment interventions for carpal tunnel syndrome can include:
- Hand splinting – helps keep the affected wrist from moving. It can also help ease the nerve compression inside the tunnel.
- Anti-inflammatory medications – can be taken orally or can be injected into the carpal tunnel space to help minimize the swelling.
- Exercise – strengthening and stretching exercises can be beneficial for patients whose symptoms have gotten better. The exercises are best recommended and supervised by a competent occupational or physical therapist.
- Worksite changes – changing the position of the computer keyboard and making other ergonomic changes has been known to help ease some of the symptoms.
- Carpal tunnel syndrome surgery – eases the nerve compression in the carpal tunnel.