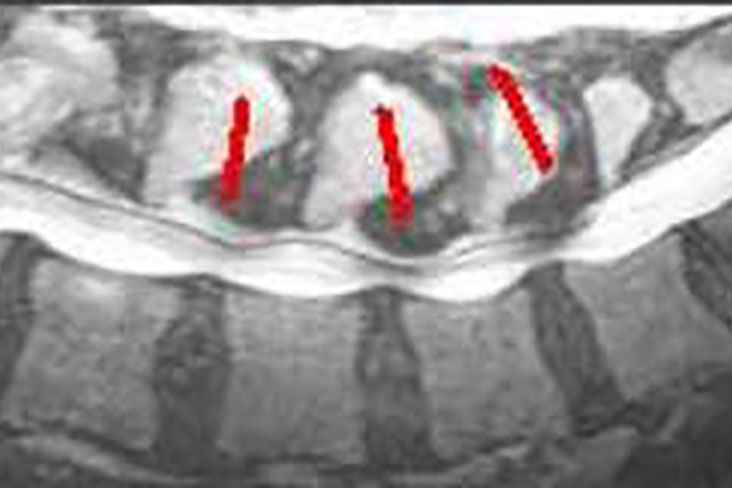
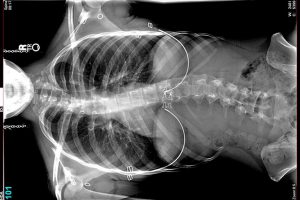
Spinal stenosis is characterized by the narrowing of the open spaces within the spine.
This narrowing can result to pressure on the spinal cord and on the nerves that pass through the spine to the legs and arms.
The condition often occurs in the neck and the lower back.
In some people, spinal stenosis will not manifest any symptoms.
However, others may experience numbness, pain, muscle weakness, tingling, and issues with bowel or bladder function.
The condition is often caused by wear-and-tear changes in the spine secondary to osteoarthritis.
In cases that are severe, surgery may be recommended in order to create additional space for the nerves or the spinal cord.
Causes
While some are born with a small spinal canal, most cases of spinal stenosis occur when the amount of space within the spine is reduced.
Other possible causes can include the following:
- Bone overgrowth – wear-and-tear damage due to osteoarthritis can result in the formation of bone spurs which can form in the spinal canal. Paget’s disease, a bone condition common among adults can also result in bone overgrowth in the spine.
- Thickened ligaments – the tough cords that help hold the bones of the spine can thicken and become stiff over time. The ligaments that are thickened may end up bulging into the spinal canal.
- Herniated disk – as one age, the soft cushions that function as shock absorbers between the vertebrae can dry out. The cracks in the exterior of the disk may cause some of the inner material to escape, causing it to press on the nerves or the spinal cord.
- Spinal injuries – vehicle accidents (and other traumas) can result in fracture or dislocation of one or more vertebrae. Bones displaced from spinal fractures can end up damaging the contents of the spinal canal. When adjacent tissues swell following back surgery, it can also cause pressure on the nerves or the spinal cord.
- Tumours – abnormal growths can also develop inside the spinal cord (in the space between the vertebrae and the spinal cord or within the membranes covering the spinal cord).
Symptoms
While spinal stenosis may be evident on X-rays, it is possible that no symptoms or signs will manifest.
However, when symptoms occur, they usually start gradually and get worse as time goes on.
Depending on the location, symptoms of the condition can vary.
- Lower back (lumbar spine) – when the nerves in the lumbar spine are compressed, it can result in leg pain or cramping (especially when walking or standing for prolonged periods). In most cases, discomfort is eased when the patient sits down or bends forward.
- Neck (cervical spine) – weakness, tingling, and numbness in the foot, arm, hand, or leg are some of the most common symptoms that signal cervical stenosis. While tingling in the hand is considered the most prevalent, many patients also report balance and walking issues. Bowel or bladder nerves may also become affected, resulting in incontinence.
Visiting an orthopaedic specialist is recommended if there is persistent numbness, weakness, and pain in the legs, back, and arms.
Complications
While rare, untreated cases of spinal stenosis may cause long-term:
- Weakness
- Numbness
- Balance issues
- Paralysis
- Incontinence
Pain Management and Treatment
Treatment intervention and pain management for spinal stenosis will vary and will depend on the severity of the symptoms and the location of the stenosis.
Medications
To help ease pain caused by spinal stenosis, the following may be prescribed:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) – minimizes inflammation and relieves pain associated with osteoarthritis.
- Antidepressants – to help alleviate chronic pain, nightly doses of tricyclic antidepressants may be recommended.
- Muscle relaxants – cyclobenzaprine (Fexmid, Amrix) can help calm muscle spasms associated with spinal stenosis.
- Anti-seizure drugs – to ease pain due to damaged nerves, anti-seizure drugs such as pregabalin (Lyrica) and gabapentin (Horizant, Gralise, Neurontin) may be prescribed.
Physiotherapy
There is a tendency for some patients with spinal stenosis to become less active in an effort to alleviate the pain.
However, it can prove counterproductive as it can result in muscle weakness which causes more pain.
Fortunately, a physical therapist can recommend exercises that can help:
- Build up the patient’s endurance and strength
- Retain the stability and flexibility of the spine
- Improve the patient’s balance
Surgery
Surgery might be recommended if conservative treatment interventions have proved futile or if the patient has been disabled by the symptoms.
The primary goal of the procedure would be to relieve nerve roots or spinal cord pressure by creating space within the spinal canal.
- Laminectomy – This procedure involves the removal of the lamina (back part) of the vertebra affected. To maintain spine strength, the vertebra may have to be linked to the adjoining vertebrae with a bone graft (spinal fusion) or metal hardware.
- Laminoplasty – This procedure is only carried out on the vertebrae found in the neck. By creating a hinge on the lamina, the space within the spinal canal is opened up. The gap in the spine’s opened section is bridged using metal hardware.
- Laminotomy – This procedure involves removal of just a portion of the lamina, with a hole carved just big enough to relieve pressure in a certain spot.