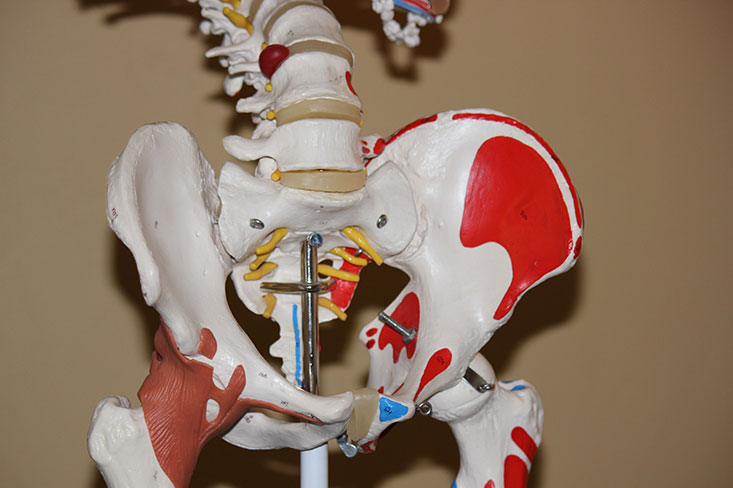
As with most types of chronic pain, women tend to experience hip aches more often than men.
While hip pain can be attributed to different things, identifying the correct cause is important so the best treatment intervention is given. To ensure the diagnosis is correct, orthopaedic surgeons need to make sure the problem is really in the hip. In some cases, women complain about hip pain when what they really have is a pain in the upper buttock, lower back, the side of the thigh and even in the knee. This is known as “referred” pain. Hip pain is often experienced on the outside of the hip (directly over the hip joint) or in the groin.
Likely Causes
When a patient visits the doctor for hip pain, key factors—age, activity level, build, etc.—are taken into consideration to help accurately diagnose the condition. Understandably, depending on if the patient is a 20-something runner or a sedentary and heavy 80-year-old, the likely causes can differ significantly. Below are some of the most prevalent causes of hip pain in women:
Arthritis
Simply put, arthritis is the inflammation of the joints. The condition can affect only one joint or multiple joints. There are more than 100 different types of arthritis, with different causes and treatment interventions. Rheumatoid arthritis (RA) and osteoarthritis (OA) are considered two of the most common types.
Causes
The cartilage is the firm and flexible connective tissue found in the joints. It works by protecting the joints by absorbing the shock and pressure when there is stress or when you move. A reduction in the normal amount of cartilage tissue can cause the condition to manifest.
Symptoms
Stiffness and joint pain are some of the most common indicators of arthritis. Decreased range of motion may also manifest when climbing, getting in and out of a chair or car or when squatting. Many patients notice that the symptoms are often worse in the mornings, this being called “start-up” pain.
Treatment
The primary goals of the treatment include minimizing the pain and preventing further joint damage. A combination of treatment methods—medications, physical therapy, and surgery—might be recommended to achieve the best results.
Bursitis
The fluid-filled sacs or saclike cavities that help minimize the friction over the body’s bony prominences are called the bursae. The inflammation of the bursae is called bursitis. At the hip, it is situated over the widest part known as trochanteric bursitis. When inflamed, it can cause discomfort and pain in the joint affected. It can also limit joint movements or a “snap” can be felt.
Causes
Bursitis is often attributed to damage or injuries to the bursae. However, different causes have been identified, depending on the type of bursitis.
In the trochanter, it can be traced to friction, injury, infection, improper posture and other diseases that affect the bones like arthritis. In rare instances, gout needs to be excluded.
Symptoms
Telltale indicators of bursitis include swelling, redness, pain, and thickening of the bursae.
Treatment
Pain medications, icing, and rest may help relieve some of the symptoms of the condition. The iliotibial band overlying the trochanteric must be stretched.
However, other treatments might be recommended, such as:
- Antibiotics – necessary when there is an infection.
- Corticosteroids – given to relieve swelling, inflammation, and pain.
- Physical therapy – helps relieve pain and other symptoms.
- Surgery – might be necessary when there is a need to drain fluids or remove the damaged bursae.
Femoral Hernia
The muscles are usually strong enough to keep the organs and intestines in their proper place. However, when you overstrain, a portion of tissue is pushed through the wall of the femoral canal. This can result in a condition known as femoral hernia. The condition is also referred to as femorocele.
Causes
The exact cause of femoral hernia (and other hernias for that matter) is often unknown. The patient may be born with a weakened femoral canal or the area might become weak over time. The weakening of the muscle walls is also attributed to straining. Several factors have been known to lead to straining, including chronic constipation, heavy lifting, childbirth, obesity and chronic coughing.
Symptoms
Small to moderate-sized femoral hernias often do not manifest any symptoms. Large hernias may be more noticeable and may cause discomfort. A bulge may also manifest in the groin area near the upper thigh. Left untreated, the condition may sometimes lead to other problems especially if the hernia blocks and obstructs the blood flow to the intestines. This condition is called strangulated hernia and will require prompt surgery.
Treatment
Asymptomatic and small femoral hernias may not require specific treatment. However, the doctor might need to monitor the condition until the symptoms progress. Moderate to large-sized femoral hernias will require surgical repair.
Sciatica
The sciatic nerve begins at the spinal cord, runs through the buttocks and hips, and branches down to each leg. The sciatic nerve is one of the longest nerves in the body and is also considered one of the most important. When irritated, it can lead to a condition known as sciatica.
Causes
Sciatica is caused by an underlying pressure or injury to the sciatic nerve. At the late stages of pregnancy, the baby’s position in the birth canal may press on roots of the nerve. A slipped disc in the spine is also a common cause of sciatica. It is common among people between 30 to 50 years of age.
Symptoms
Pain that flows from the lower back area through the buttock area and into the lower limbs often signals sciatica.
Other symptoms include:
- Pain that gets worse with movement.
- Weakness or numbness in the legs or feet.
- Pins and needles sensation or painful tingling in the feet or toes.
- Inability to control the bowel or bladder.
Treatment
For mild cases, at-home treatments like OTC medications, stretching, and using hot or ice packs will suffice. However, if the condition does not respond to home care remedies, other treatment alternatives like physical therapy, prescription medication, and epidural steroid medication might be recommended. An MRI or CT scan may be indicated. Surgery might be resorted to when there is incontinence or severe pain or leg weakness.
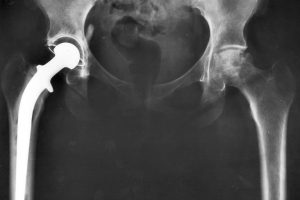
Hip Fractures
A fracture in the upper quarter of the thigh (femur) bone is called a hip fracture. The extent of the break will often depend on the forces involved. Surgery to treat a hip fracture will be based primarily on the soft tissues and bones that are affected as well as the level of the fracture.
Causes
Hip fractures often occur from direct blows to the side of the hip or from falls. However, some medical conditions like cancer, stress injuries, and osteoporosis can also weaken the bone and can make the hip bone more prone to breaking.
Symptoms
Patients with a hip fracture will often experience pain in the groin or the outer upper thigh. Significant discomfort may also be felt when rotating the hip or flexing. It is usually impossible to bear weight. If the bone has been weakened by diseases like cancer, patients might experience aching in the thigh or groin area for a period of time before the bone breaks. If the bone is completely broken, the injured leg may appear shorter compared to the non-injured one.
Treatment
Once the diagnosis has been made, the overall medical and health conditions of the patient will be evaluated. In some cases, patients might be very ill that surgery will not be recommended. In similar scenarios, the level of pain and overall comfort of the patient will be weighed against the risk of anaesthesia and surgery. Few fractures are deemed stable enough to be managed with nonsurgical treatment. This will be those involving the trochanter alone which does not support the body weight.
However, since there is still the risk that these stable fractures can become displaced (change position) and unstable, periodic X-rays of the area will be recommended. If bed rest will be suggested as part of the management of the fracture, close monitoring is advised so complications from prolonged immobilization will not develop. Possible complications can include pneumonia, bedsores, infections, nutritional wasting, and blood clot formation.